Overview
Apollo AyurVAID’s Stroke Rehabilitation Program offers a comprehensive, evidence-based approach to help stroke survivors regain mobility, speech, cognition, and emotional well-being.
The goal is to increase the efficiency of functional independence of daily life activities and improve the quality of life.
With stroke incidence rising—especially among younger adults—early, structured stroke recovery programs are essential to prevent long-term disability and dependency.
In Ayurveda, stroke is referred to as Pakshaghata—‘Paksha’ meaning one side of the body, and ‘Aghata’ indicating injury or paralysis. It is classified as a Vata Vyadhi, caused by an imbalance of Vata Dosha, which governs movement and neural activity.
Pakshaghata is broadly categorised into:
Dhatukshayajanya – Caused by chronic Vata aggravation and degeneration of Majja Dhatu (nervous tissue), common in the elderly or those with diabetes, hypertension, or neurodegenerative conditions.
Avaranajanya – Due to Marga Avarana (obstruction of Vata) by Kapha, Pitta, or Ama, presenting with acute stroke-like symptoms, especially ischemic.
Stroke survivors often face recovery challenges such as neuroinflammation, impaired blood-brain barrier function, and secondary issues like anxiety, fatigue, sleep disturbances, and digestive problems.
The Apollo AyurVAID Integrative Stroke Rehabilitation Program Blends Precision Ayurveda with modern therapies like physiotherapy, speech, and occupational therapy to address both root cause and symptoms. Ayurveda Stroke Treatment (integrative) has a comprehensive approach that promotes faster neurological recovery and improved functional outcomes compared to conventional care alone.
Why Opt For AyurVAID’s Integrative Stroke Rehabilitation?
Ayurveda Stroke Rehabilitation approach at Apollo AyurVAID is –
- Personalised and Protocol-Driven – taking a comprehensive, protocol-driven approach, targeting the root cause of disease instead of merely symptoms, to give a natural path of recovery.
- Multidisciplinary and Non-Conflicting– Our treatment regimen fully integrates with your ongoing stroke care. We will work closely with your neurologist, dietitians, and physiotherapists.
- Regular Monitoring and Updates- The measurement of progress is done through standardized scales and timely laboratory assessments. Regular follow-ups and updates are provided to the primary neurology team.
Who Can Benefit and Who May Not: AyurVAID’s Integrative Stroke Rehabilitation Scope
Who Can Benefit:
- Medically Stable Patients: Patients with stable vital signs for whom acute care has been provided.
- Patients in the Early or Moderate Phases of Stroke Recovery: Reap maximum benefit by improving motor-sensory and cognitive recovery with integrative modalities.
- Post-Stroke Deficits: Individuals with residual physical deficits (i.e, weakness, stiffness) are likely to respond well to integrative therapies.
- Individuals Seeking Overall Recovery: An extended plan for full recovery, including physical, emotional, and psychological recovery.
- Patients With Comorbidities: Patients with other conditions like diabetes or hypertension.
Who May Not Benefit:
While integrative rehabilitation is essential for all stroke patients, certain individuals may require additional medical precautions:
- Medically Unstable Patients: Patients with unstable vitals and who present with severe comorbidities must be medically stabilized before undergoing rehabilitation.
- Patients with Severe Cognitive Decline: Those having difficulty with engagement and participation in standard therapies and protocols are not enrolled. They may require specific tailored interventions that would come before the rehabilitation process.
- An Unsupportive Environment: Effective rehabilitation requires a supportive environment, and an adequately supportive caregiver must be assured.
When should AyurVAID’s Integrative Stroke Rehabilitation Begin?
Stroke rehabilitation begins as soon as the acute phase of the stroke is stabilized, thereby ensuring the patient is medically stable. In general, rehabilitation begins 7 to 10 days after the acute phase, after the individual’s vital signs are stable and they can tolerate therapy.
Research demonstrates that the most substantial recovery following a stroke is generally observed within the first three months of a rehabilitation program (‘Golden Period of recovery’). However, recovery may continue beyond this initial period and up to 6-8 months following an episode of stroke.
Evidence suggests that the prompt initiation of rehabilitation services is associated with improved outcomes, enabling individuals to reintegrate successfully into their professional and social environments. Furthermore, Ayurveda therapies offer natural ways to regain strength, resilience, and peace of mind even in patients who have had residual complications due to a stroke for longer than one year.
How Long Should AyurVAID’s Integrative Stroke Rehabilitation Last?
The success of rehabilitation services and functional recovery in post-stroke cases is determined by specific factors, such as age (recovery is comparatively slower in the elderly), site and extent of stroke, nature of the stroke (ischemic or hemorrhagic), patient’s lifestyle until just before the stroke episode (an active lifestyle usually shows better recovery), and comorbidities.
In general, rehabilitation typically lasts 21 to 45 days, with follow-up appointments every 3 to 6 months or more.
What Caregivers Can Expect from AyurVAID’s Approach
AyurVAID follows a protocol-driven, highly individualized and integrative approach whereby it addresses physical signs of disease along with identifying the underlying physiological and systemic barriers to recovery, which are often neglected, such as:
- Neuroinflammation– sustained inflammation causing cell death in the nervous system, thereby delaying brain recovery.
- Impaired Blood-Brain Barrier (BBB) Function: A stroke weakens the BBB, reducing the delivery of nutrients and oxygen to the healing brain tissue.
- Secondary Health Issues: Anxiety, mood disorders, and exhaustion impair the rehabilitation process.
- Circadian Rhythm Disruption: Disturbances in sleep and the gastrointestinal tract, such as constipation, can adversely affect rehabilitation in total.
How AyurVAID Supports Recovery
- Chronic inflammation and oxidative stress are alleviated through detoxification and balancing doshas.
- Restores normal metabolism through gut health restoration, digestion, and holistic support for neuroplasticity.
- It regulates sleep, bowel, bladder, and oro-motor activities to help patients regain independence.
- Mind-body wholistic care improves emotional resilience and cognitive clarity.
Integrating Approach: How Therapies Work Together
The integration of Ayurveda treatment with other treatment modalities (physiotherapy, speech, and occupational therapy) synergistically addresses common deficits and limitations following stroke.

Common Impairments After Stroke:
- Gait, balance, and mobility
- General pain, stiffness, and spasticity
- Upper limb and shoulder function
- Cognition
- Vision
- Speech
- Nutrition
- Dysphagia
- Continence
General Rehabilitation Principles (Conventional)
Early Mobilization
- Patients should be mobilized as early as medically possible.
- Minimizes the complications of pneumonia and pressure sores while maximizing muscle strengthening, cardiovascular health, and respiratory functioning.
Therapeutic Positioning
- Aids in muscle tone regulation, sensory input improvement, and complication prevention.
- Patients should be placed in the upright sitting position as soon as possible (if their medical condition allows), as it helps improve oxygen saturation.
Personal ADL Training by Occupational Therapists
- Focuses on self-care tasks like grooming, dressing, feeding, and toileting.
General Rehabilitation Principles (Ayurveda)
Stabilize and Balance Vata and Other Doshas
- Therapies are customized based on individual constitution and disease stage.
Nervous System Nourishing
- Ayurveda Stroke treatments create a conducive neurochemical environment, creating favorable conditions for physiotherapy and speech therapy.
- Continuous feedback among therapists.
Improves Muscle Tone and Circulation
- Ayurveda helps reduce muscle spasticity and rigidity, while physiotherapy helps build strength and improve coordination.
- Occupational Therapy ensures that this strength translates into functional independence.
Gut-Brain Axis Restoration
- Ayurveda helps improve digestion and metabolism (Agni) for systemic healing and neuroplasticity.
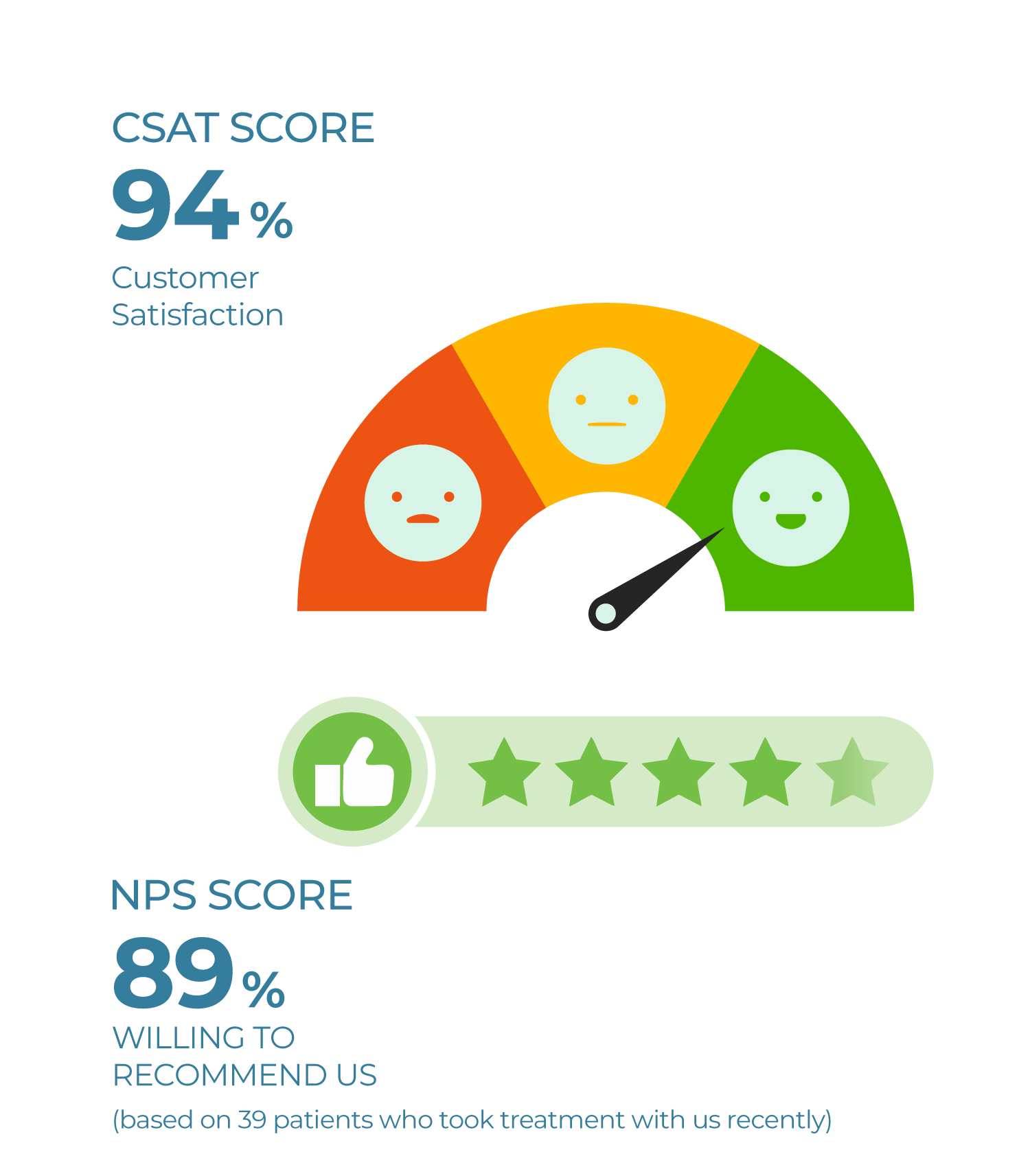
Patients highly rate our Clinical Care, Outcomes, and Service
Patients expressed high satisfaction with their Psoriasis treatment, highlighting significant improvements in their conditions.
AyurVAID’s 4-Step Approach to Determine Root Cause and Create Individualized Treatment Plan
At Apollo AyurVAID, we create a personalized four-step cyclic approach to stroke recovery that integrates Ayurveda with modern neurological rehabilitation. The four steps are Assessment, Goal Setting, Personalized Care, and Reassessment. Patients are helped to achieve independence, manage recurrence, and have a better quality of life.
- Disease Assessment as the Understanding of the Whole Person
Our Ayurveda physicians conduct tests, such as Ashta Sthana Pariksha, Dasha Vidha Pariksha, Srota Pariksha, and Nidana Panchaka, to analyze the underlying cause and root imbalances. These tests are combined with brain imaging, ECGs, blood pressure readings, and laboratory investigations to give a complete picture. Based on the affected doshas, srotas, and tissues, a “disease tree” is created. The Shatkriyakala (six stages of disease) model is applied to determine the stage of the disease and the extent to which it can be reversed, stabilized, and rejuvenated. - Goal Setting
Realistic and clear short- and long-term goals are set with the patient and caregivers. - Personalized, Protocol-Based Care Plan
Every patient receives personalized and tailored care combining Ayurveda with modern rehabilitation therapies. - Re-assessment
Progress is periodically monitored using globally recognized assessment scales to ensure the effectiveness of therapies and adjust the care plan as needed. Some standard scales include: Fugl-Meyer Assessment (FMA): Motor recoveryBarthel Index (BI): Everyday activity independence Modified Rankin Scale (mRS): Overall disability Modified Ashworth and Tardieu Scales (MAS and MTS): Muscle tone & spasticityBerg Balance Scale (BBS): Postural control & risk of fallingFunctional Independence Measure (FIM): Level of disability and patient’s response to rehabilitation or medical intervention.
AyurVAID’s Protocol-Driven Integrative Stroke Rehabilitation
A Targeted Approach to Post-Stroke Recovery: Restoring Independence and Reviving Quality of Life
At AyurVAID, we bring about an integrative program of post-stroke rehabilitation stroke rehabilitation to help people restore independence, dignity, and functionality by addressing physical, neurological, and systemic challenges that follow a stroke.
A joint objective in stroke rehabilitation is to enable self-care or perform daily activities independently, or carry out Activities of Daily Living (ADLs): taking a bath, dressing, eating, toileting, and moving independently. This means allowing the most significant measure of autonomy in everyday tasks, thus increasing personal confidence and psychological well-being and reducing the emotional and physical burden on caregivers.
Localized Rehabilitation Focus (Roga Shamana)
Our rehabilitation framework focuses on treatments designed to reduce muscle rigidity, increase neuromuscular coordination, and rebuild strength and control, facilitating patients’ performance of self-care tasks in an easier, more confident way; the aim is to support independence and functional recovery.
Systemic Recovery Support (Roga Shanti)
Our approach to rehabilitation will emphasize restoring internal physiological homeostasis, enhancing cognitive clarity, and energizing systems. By taking care of the internal environment, we mitigate secondary complications during physical rehabilitation; thus, we provide a platform for a more sustainable recovery and long-term wellness
Phased and Adaptive Care Delivery
Rehabilitation has different but interrelated phases. They include the following:
- Initial Stabilization and Preparation: It is directed toward soothing the nervous system, correcting internal imbalance, and strengthening the patient. Some of the expected treatments include Abhyanga (Oil therapy), Lepa (Paste application), Dhara (Pouring of medicated liquid), and Talam(Medicated paste/ oil on head).
- Core Therapeutic Phase: Once the patient is stable and responsive, the focus will shift to deep systemic cleansing, rejuvenation, and physical therapy. This stage targets the root causes of dysfunction, supports neuromuscular recovery, and helps restore voluntary motor control. These include Snehapana (internal oleation), Virechana (Purgation), Vasti (Enema) with or without external therapies, such as Abhyanga, Rooksha Kizhi (dry herbal pouch massage), Dhara.
- Strengthening and Rehabilitation: The last phase focuses on rebuilding strength, endurance, and cognitive function. It includes measures to nourish the body, improve neuroplasticity, and support reintegration into daily life, including occupational and social roles.
Each phase is specifically tailored for that person’s state and disease condition. Their medical history and response to therapy are taken into consideration. Our team continuously monitors progress and makes necessary changes to the plans to ensure the best outcomes.
Duration of Treatment: Individualized and Evolving
For the majority, rehabilitation is a comprehensive program lasting from 3 to 8 months, while patients with more complicated or severe impairments may go for longer-term care.The duration of the program varies depending on several key factors:
- The severity and type of stroke
- Pre-existing conditions and overall vitality
- Level of neurological and physical impairment
- Response to treatment and rehabilitation progress
Our approach is not time-bound, but outcome-driven, adapting dynamically to ensure that each patient experiences progressive and sustainable improvement.
Holistic, Integrative, and Evidence-Informed
AyurVAID’s integrative stroke rehabilitation is based on classical Ayurveda principles while adhering to current clinical guidelines for neurological recovery. Our protocol-driven approach provides constant quality care, yet our deep personalisation acknowledges the uniqueness of each patient’s journey.
We help people recover and thrive by combining physical, neurological, and systemic therapy to restore function, confidence, and quality of life.
Outcomes Delivered
The Apollo AyurVAID approach to stroke rehabilitation is a systematic, protocol-based approach with measurable outcomes and sustainable recovery. The following tools and methods are adapted for treatment and outcome monitoring to establish baselines and measure improvements over time –
1. Disease-specific Scales: Progress is tracked using comprehensive assessment tools that measure multiple aspects of stroke recovery.
We use the National Institutes of Health Stroke Scale (NIHSS) and the Fugl-Meyer Assessment (FMA) to evaluate neurological and motor function.
Functional independence is assessed through the Barthel Index (BI) and the Functional Independence Measure (FIM).
The Modified Rankin Scale (mRS) evaluates the overall disability level.
Specific impairments are quantified using the Modified Ashworth Scale (MAS) for spasticity, the Modified Tardieu Scale, and the Berg Balance Scale (BBS) for balance.
The Stroke-Specific Quality of Life Scale (SS-QOL) and the Stroke Impact Scale (SIS) measure the impacts on quality of life. These standardized scales enable objective measurement of progress and provide quantifiable evidence of treatment effectiveness.
2. Biomarkers and Imaging Techniques: To assess progress and improvements.
3. Patient-Reported Outcomes: To track improvement while maintaining transparency and avoiding bias.
Key Performance Highlights for Stroke-Rehabilitation Treatment at AyurVAID
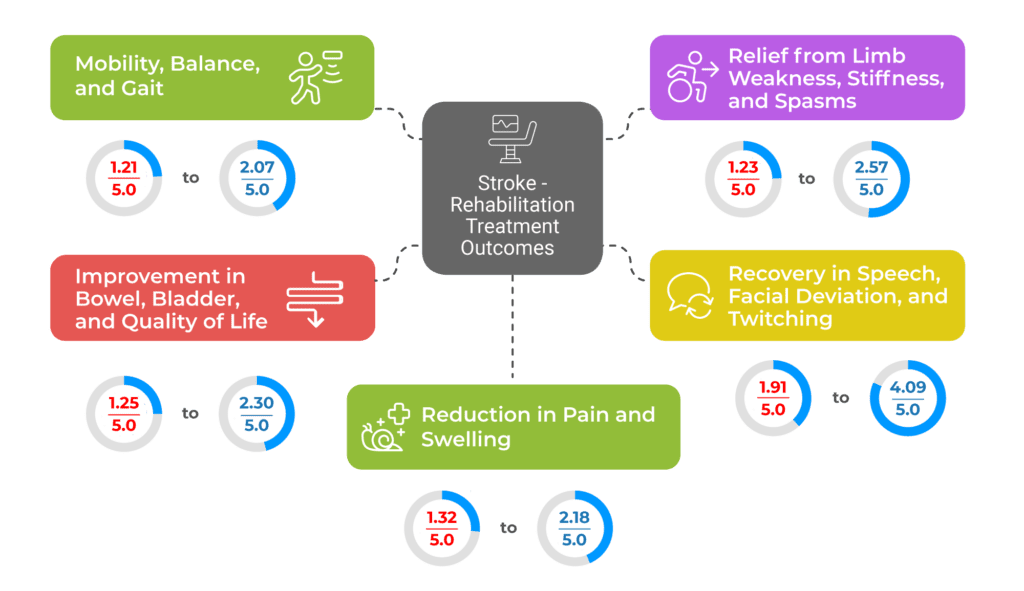
Data derived from 29 patient-reported outcome measures (PROMs) collected across AyurVAID centers.This data is representative; individual outcomes may vary. Measured using validated symptom scales and standardized PROM tools.
Case Studies
Case 1: A 59-year-old male patient with a 3-month history of Spinocerebellar Ataxia
Case Summary:The patient presented with an imbalance while walking associated with giddiness and stiffness. His gait was affected by increased imbalance during postural changes, lasting over 10 minutes and reducing on rest.
The initial assessment revealed a positive heel-shin test, tandem walking, finger-nose test, and Romberg's sign, with the stiffness of quadriceps muscles and circumduction walking. MRI showed tiny gliotic changes in the right corona radiata and cerebellar hemispheres with chronic ischemic changes. The initial SARA score was 14, and the FIM & FAM score was 193.
The patient underwent a 21-day intensive Ayurvedic treatment including external therapies (Sarvanga Utsadanam, Dhanyamladhara, Shiropichu, Churna Pinda Swedanam), specialized procedures (Kalavasthi, Nasyam), and internal medications. Post-treatment, significant improvements were noted with the SARA score reducing to 5 and the FIM & FAM score improving to 208. There was marked improvement in gait balance, speech clarity, and energy levels, with resolution of most neurological signs and symptoms.
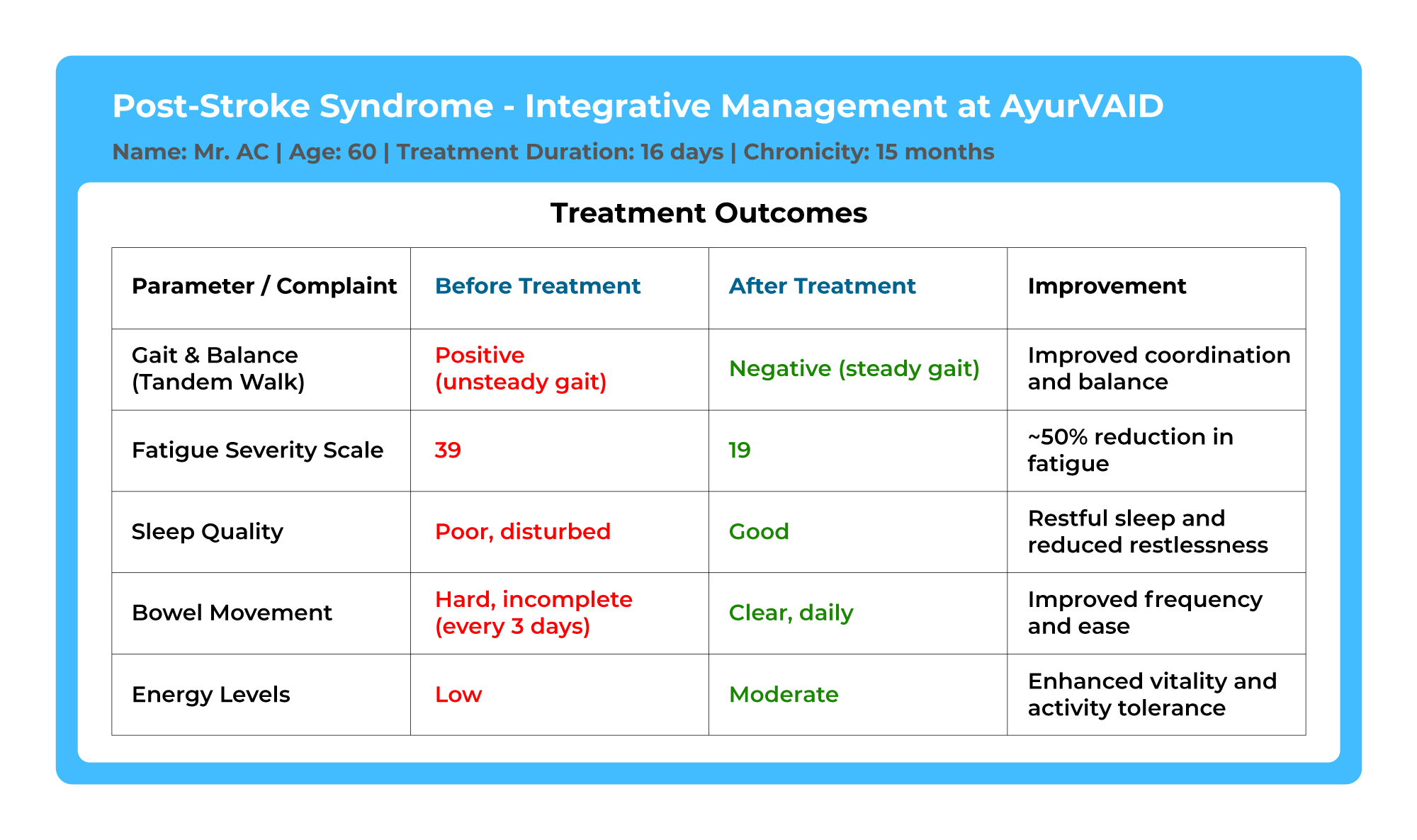
Case 2: A 60-year-old male patient with post-stroke syndrome and peripheral neuropathy
Case Summary: The patient presented with disturbed sleep and restlessness at night, low energy levels, incomplete bowel evacuation, and numbness in both soles and palms for 2-3 months, along with a recent weight loss of 3kg. He had a history of brain stroke in December 2021, after which he developed a gait imbalance and sensory symptoms.
The initial assessment revealed a positive tandem walking test, poor sleep quality, irregular appetite, and hard bowels with incomplete evacuation. He also had urinary incontinence and drowsiness. The initial SARA scale score was 3, and the Fatigue Severity Scale score was 39.
The patient underwent a 15-day intensive Ayurvedic treatment including external therapies (Sarvanga Utsadana with Bashpa Sweda, Sthanika Dhanyamladhara), specialized procedures (Samana Snehapana, Virechana, Yoga basti program, Sirodhara), and internal medications. Post-treatment, significant improvements were noted with the SARA score reducing to 2 and the Fatigue Severity Scale score improving to 19. There was marked improvement in sleep quality, bowel habits, appetite, and energy levels, with a negative tandem walking test and overall better well-being.
Scientific Evidence For Ayurvedic Stroke Recovery and Rehabilitation
- Lived Experiences of Stroke Survivors Undergoing Ayurvedic Rehabilitation Therapy in India; 2020, Research Article: Patients appeared to benefit not only in domains of self-efficacy but also in positive health behaviors and emotional well-being. The holistic approach of Ayurvedic treatment and the favorable social and emotional climate of the facility were well received. It is worth noting that this study focused on the lived experiences and perceptions of patients.
- A prospective study on the effects of Ayurvedic massage in post-stroke patients; 2019, Research Article: This prospective study investigated the effects of Ayurvedic massage in addition to standard physiotherapy on post-stroke patients compared to physiotherapy alone and found that the group receiving Ayurvedic massage achieved standing with minimal assistance sooner, had better locomotion at discharge, and showed a lower need for antispastic drugs. The researchers concluded that Ayurvedic massage could promote faster functional gains in post-stroke patients with flaccidity.
- Sameerpannag Ras Mixture (SRM) improved neurobehavioral deficits following acute ischemic stroke by attenuating neuroinflammatory response; 2017, Research Article: This study investigated the neuroprotective effects of Sameerpannag Ras Mixture (SRM), an Ayurvedic formulation, on neurobehavioral deficits and neuroinflammation in a mouse model of acute ischemic stroke. The researchers found that SRM treatment significantly improved neurological function and motor skills in mice post-stroke by attenuating the expression of key inflammatory genes and proteins. This suggests that SRM has the potential to be a therapeutic agent for ischemic stroke by suppressing the neuroinflammatory response.
- Antioxidant/restorative effects of calcined gold preparations used in Indian systems of medicine against global and focal models of ischaemia; 2002, Research Article: This study investigated the potential antioxidant and restorative effects of two Indian traditional medicine gold preparations, Swarna Bhasma and Kushta Tila Kalan, in rat models of global and focal ischaemia (stroke). The findings indicate that oral administration of both preparations significantly reversed the ischaemia-induced alterations in enzymatic parameters associated with oxidative stress, suggesting their potential therapeutic role in cerebrovascular diseases. The observed biochemical improvements also correlated with positive histopathological changes in the brain tissue.
- Evaluation of Antioxidant and Cerebroprotective Effect of Medicago sativa Linn. against Ischemia and Reperfusion Insult; 2011, Research Article: This study evaluated the antioxidant and cerebroprotective effects of Medicago sativa (MS) against ischemia and reperfusion injury in a mouse model of stroke. The findings showed that pre-treatment with MS significantly reduced cerebral infarct size, decreased oxidative stress markers, and improved neurological function. The study suggests that MS has neuroprotective potential due to its antioxidant properties.
Hear from our patients!
“I had been suffering from severe shoulder pain since my stroke in 2019, with pain levels reaching up to 100%. After just 20 days of Ayurveda treatment at AyurVAID, the pain came down to 20%. I never knew about this treatment before, but now I’ve truly experienced its benefits. I would definitely recommend Ayurveda to anyone in a similar situation.”
Mr. JCZ
“After my aneurysm, I was completely dependent — I couldn’t walk or move my right side. In the US, therapy was limited. But at AyurVAID, with their integrated approach and intensive therapy — twice-daily physio, Ayurveda sessions, and speech therapy — I can now walk alone, move my right hand almost fully, and live independently. This place gave me back my life.”
Mr. N
Frequently Asked Questions (FAQs)
References
Did the information meet your needs?
As we work hard to improve our services, your feedback is important to us. Please take a moment to help us serve you better.
Disclaimer
The information provided in this blog is for general informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician, Ayurvedic practitioner, or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment.
Stay Connected to Health and Wellness
Subscribe to our hospital newsletter for the latest health tips, updates on services, patient stories, and community events. Sign up today and stay informed!
Ayurveda Doctors for Stroke Rehabilitation




Dr. Bheema Bhatta

Related Blogs

- Read More








